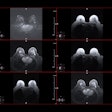
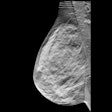
Lymphosonography can detect sentinel lymph nodes (SLNs) in cervical and vulvar cancer patients scheduled for surgery, suggest findings presented March 30 at the 2025 American Institute of Ultrasound in Medicine (AIUM) annual conference.
Priscilla Machado, MD, from Thomas Jefferson University in Philadelphia, shared results from research demonstrating that this ultrasound method led to more than 90% of SLNs being identified.
“I believe that this technique can improve patient care by providing a way to perform biopsy in the SLN even if clinically they don’t look suspicious,” Machado told AuntMinnie.com. “That way, the surgeons can know beforehand if there is SLN involvement that hopefully would decrease the number of patients that have to undergo unnecessary SLN excision.”
 Priscilla Machado, MD, presents her team's research at AIUM 2025, showing how lymphosonography can be a useful tool in assessing sentinel lymph nodes (SLNs) in women with cervical or vulvar cancer.
Priscilla Machado, MD, presents her team's research at AIUM 2025, showing how lymphosonography can be a useful tool in assessing sentinel lymph nodes (SLNs) in women with cervical or vulvar cancer.
SLNs are the first nodes in the lymphatic chain, meaning that if these nodes are free of cancer cells, the rest of the lymphatic chain is also free from metastatic disease.
Surgical excision is the standard for assessing lymph nodes in cervical or vulvar cancer patients. However, Machado said this has its limitations and can affect SLN detection and accuracy for disease staging.
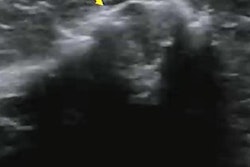
Lymphosonography is a contrast-enhanced ultrasound (CEUS) method that can localize SLNs and provide lymphatic mapping data. Machado said this method has several advantages, including not requiring ionizing radiation, having better spatial resolution and anatomical delineation, and portability.
Machado and colleagues evaluated lymphosonography’s potential as an alternative to surgery for women with cervical or vulvar cancer. In this study, five patients who were scheduled for SLN excision underwent this procedure. This included contrast agent administration in four parts at different positions surrounding the primary tumors. Each part had 0.25 ml of contrast administered, making for a total of 1 ml administered.
Machado reported that 11 SLNs were surgically removed from the women. Three of the women had cervical cancer, with eight iliac SLNs being the nodes removed and sent to pathology. Of these, six were benign while two were malignant.
The remaining two patients had vulvar cancer, with three inguinal SLNs being removed and sent to pathology. Two of these SLNs were deemed benign while the other one was malignant.
Lymphosonography meanwhile identified 17 SLNs in the five women. Compared to the surgically removed SLNs, lymphosonography found 10 of these (91%). It also found all benign SLNs and two of the three malignant SLNs.
“The most surprising thing was how the midline location of tumor doesn’t really translate to a bilateral SLN drainage in the majority of the cases,” Machado said.
Machado said the results indicate that lymphosonography can be used to identify SLNs, which is an important aspect of predicting outcomes for patients with cancer, albeit based on a small sample size.
She said that more cases are needed to validate the team’s findings.
“We are working on future grants where we will expand the areas that we will study,” Machado told AuntMinnie.com. “For instance, we want to move to get studies done in melanoma, head and neck cancers, lymphedema and to continue the studies in breast, esophageal, cervical, and vulvar cancers.”